A strong, thick band of tissue called the plantar fascia runs along the bottom of your foot and connects your heel bone to your toes. The plantar fascia helps support the arch of your foot and absorbs shock when you walk, run or jump.
Plantar fasciitis is diagnosed when your plantar fascia is swollen or damaged. The main symptom is heel pain. Your heel may hurt more in the morning, after sitting or standing for a long time, or after heavy exercise.
Plantar fasciitis can affect your daily life and make simple actions like walking hard. Summit Orthopedics experts in the Minneapolis/St. Paul area have the expertise to diagnose and treat plantar fasciitis to relieve your discomfort as quickly as possible.
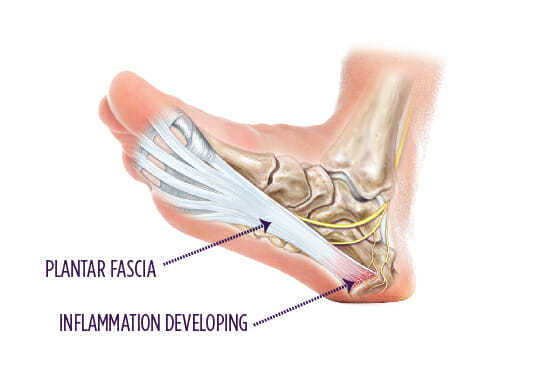
Causes of Plantar Fasciitis
Plantar fasciitis happens from overuse. Stress from activities like walking and sports can, over time, lead to pressure or small tears in your heel tissue.
A common misunderstanding is that heel spurs cause plantar fasciitis. A heel spur is a small bony growth on your heel bone. While about half of the people with plantar fasciitis also have heel spurs, these spurs are not the cause of plantar fasciitis.
How to Prevent Plantar Fasciitis
You can lower your chances of getting plantar fasciitis by following these simple tips:
- Maintain a healthy weight. Staying within a healthy weight range reduces pressure and stress on your feet.
- Stretch regularly. Regularly stretching your feet, ankles and calves helps keep the plantar fascia flexible. Stretch in the morning before getting out of bed and before and after exercise.
- Take breaks when standing. If your job requires long periods of standing, shift your position or take regular breaks. This helps reduce strain on your feet.
- Wear the right shoes. Choose shoes with good arch support and cushioning. Replace worn-out athletic shoes regularly.
Risk Factors
Several factors can make you more likely to develop plantar fasciitis. Knowing your risk helps you prevent the condition or understand why you might get it.
- Your age: Plantar fasciitis is most common in adults between ages 40 and 60. Younger adults, particularly athletes, can also get it.
- Body weight: Being overweight or gaining weight quickly adds stress to your feet.
- Foot shape: Having flat feet or very high arches can change how your foot absorbs weight. This can lead to more strain on the plantar fascia.
- Tight muscles: Tight calf muscles or Achilles tendons can change how you walk and put extra strain on your heel.
- Activities: Sports like running or dancing that involve repetitive impact can increase your risk.
- Poor shoe fit: Wearing shoes with little support or worn-out athletic shoes can also contribute to the problem.
Diagnosing Plantar Fasciitis
To diagnose your condition, your doctor will examine your foot for tenderness, swelling, and stiffness. They may also order an X-ray to rule out other issues that could be causing your symptoms, like a fracture or arthritis. This helps them confirm the diagnosis and create the most effective treatment plan for you.
When to See a Doctor
If heel pain bothers you and interferes with your daily activities, it’s a good idea to talk with an orthopedic specialist. They can help determine whether it’s plantar fasciitis or another problem. Getting the right diagnosis early allows you to treat the problem early.
Nonsurgical Treatment
Most people with plantar fasciitis get better with nonsurgical treatment. Without surgery, it can take a while to improve. The goal of these treatments is to ease pain, lower inflammation and help the plantar fascia heal.
Common nonsurgical plantar fasciitis treatments include:
- Casts: Foot casts keep your foot from moving so it can rest and heal faster.
- Calf and foot stretches: Several stretches can help improve plantar fasciitis symptoms. These plantar fasciitis stretches include leaning on a wall while keeping your feet on the floor, using a towel to stretch your foot and stretching the bottom of your foot. A physical therapist may recommend additional exercises.
- Corticosteroid injections: These injections involve inserting medication into your foot to reduce swelling.
- Ice: Rolling your foot over ice several times throughout the day is one method that may help ease symptoms.
- Medication: Ibuprofen and other nonsteroidal anti-inflammatory drugs (NSAIDs) are effective at relieving plantar fasciitis symptoms, specifically reducing pain and inflammation.
- Night splints: You wear these flexible devices on your feet. They help stretch your plantar fascia while you sleep.
- Supportive shoes: Shoes with more cushioning and thicker soles can reduce tension on your feet as they land on the ground. Your doctor may recommend getting custom shoe inserts.
Plantar Fasciitis Surgery
Your doctor may only suggest surgery if you have a lot of pain after trying all other options for at least 12 months.
There are two main types of plantar fasciitis surgery, and your surgeon will recommend one based on the cause and severity of your condition. Your surgeon will work closely with you to determine the best treatment option for your specific needs.
- Gastrocnemius recession: If tight calf muscles cause your plantar fasciitis, your doctor may suggest this surgery. In this procedure, your surgeon makes one of the calf muscles longer. This helps the ankle move better and takes pressure off the plantar fascia.
- Partial plantar fascia release: In this surgery, your surgeon makes a small cut in your heel. They then cut a part of the plantar fascia ligament to help relieve tension. Sometimes, this surgery is done alongside a gastrocnemius recession.
Expert Care for Plantar Fasciitis at Summit Orthopedics
At Summit Orthopedics, we treat plantar fasciitis with expert care, using the latest approaches. When surgery is needed, we use advanced methods. This includes minimally invasive surgery, which helps ease your symptoms and shortens recovery time.
Summit Orthopedics surgeons are available at nearly 30 convenient locations across the Minneapolis/St. Paul metro area, serving Minnesota and western Wisconsin. Our state-of-the-art, comprehensive orthopedic centers offer same-day appointments from a team of experts who offer the full scope of orthopedic care.
Find your Summit Orthopedics foot expert, request an appointment or call us at (651) 968-5201 to schedule a consultation.
